For uniformed service members, retirees, and their families in the USA, TRICARE is essential to providing comprehensive health services. TRICARE, managed by the Defense Health Agency, covers health, special programs, medicines, and dental plans.
Military insurance is about helping the US military and boosting healthcare providers’ patient bases. Providers show their dedication to military service and quality care.
Tricare Credentialing is essential for providers to meet TRICARE criteria. This checks a provider’s education, training, experience, and licensure. Providers must be qualified and experienced to provide great treatment to TRICARE beneficiaries.
This credentialing is more than a checkbox for physicians; it shows trust and credibility. It shows patients and insurance networks, including TRICARE, that providers meet high criteria and are dedicated to providing the finest care to veterans.
What is TRICARE Credentialing?
TRICARE credentialing is the process through which healthcare providers are reviewed and approved to deliver services to active duty service members, retirees, and their eligible family members. This process includes evaluating education, training, licensure, background, and professional qualifications.
The purpose of TRICARE credentialing is to ensure that providers within the network are properly qualified and capable of delivering safe, high-quality care. Because the TRICARE population includes military families with specific access needs, the standards for participation matter greatly.
For providers, successful credentialing supports both compliance and growth. It opens the door to a broader patient base while also showing that the practice is prepared to meet the expectations of a national healthcare program serving a distinct population.
Make the TRICARE Process Easier to Manage
If your practice is preparing to join the network or facing delays with documentation and follow-up, resilient mbs can help simplify Tricare Credentialing Services with a more organized and reliable process.
Steps for TRICARE Credentialing
Sending an Application
Fill out an application form and send it to TRICARE with the necessary papers for review.
Checking Your Credentials
TRICARE checks your credentials, such as your schooling, training, licenses, and certifications.
Approval Process
Once your identity has been confirmed, TRICARE will look over your application and grant your credentials if you meet their standards.
Importance for Military Family Providers
Providers need Tricare accreditation for several reasons. First, it provides access to TRICARE patients military personnel, retirees, and their families.
Second, TRICARE-authorized providers are dedicated to providing high-quality treatment to a distinct and deserving population, boosting professional reputation.
Third, joining Tricare can enhance patient referrals and income since many military families prefer Tricare-covered providers. Finally, TRICARE provides network providers training, policy updates, and claims and invoicing assistance.
TRICARE Credentialing for Behavioral Health Providers
This type of credentialing covers uniformed service members, retirees, and their families worldwide, and requires mental health providers to be credentialed. These regulations ensure providers meet care and competency standards.
Some key considerations for behavioral health credentialing with TRICARE include:
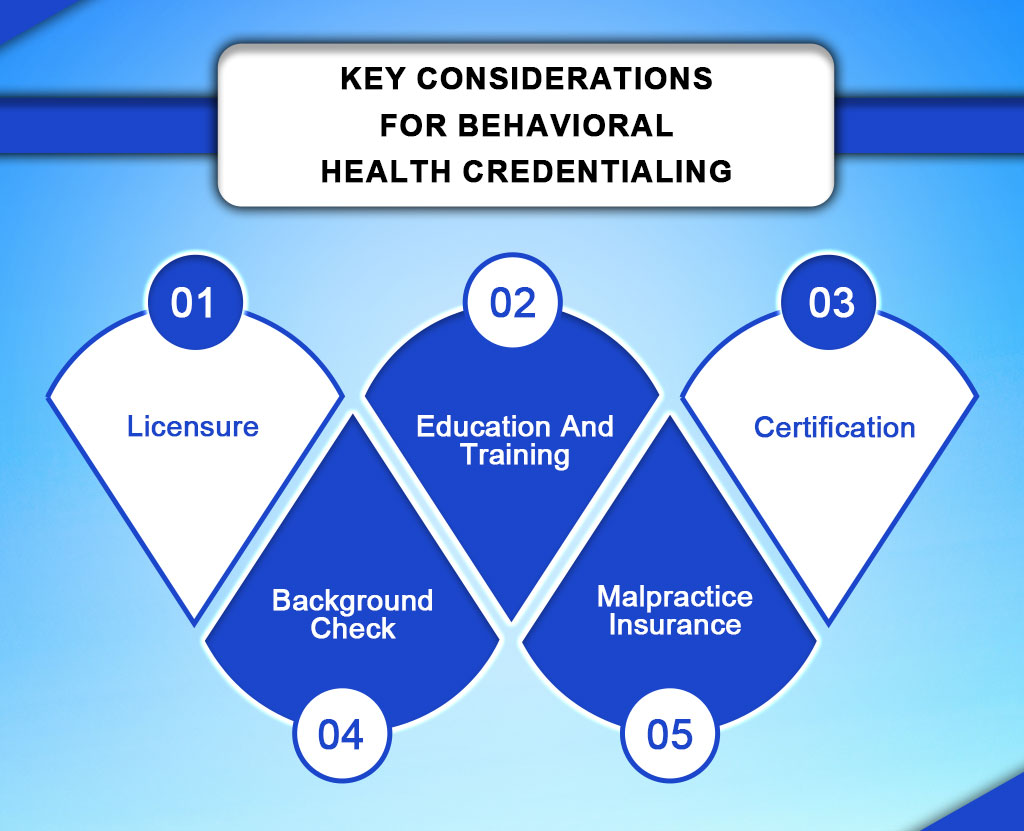
Licensure
Providers must also be current and clear to practice independent practice in their state or country. Containing the license, this agreement must correspond to the provider’s specialty and scope of practice.
Education and Training
It requires that BH professionals have appropriately completed a graduate or postgraduate program in specialty areas of practice, e.g., psychology, SW, or counseling. They should also possess proven course and vocational aptitude in handling mental health disorders.
Certification
It is important to recognize that some types of behavioral health providers, depending on their specific scope of practice, may require other forms of certification and/or licensure, which may include board certification in psychiatry or as an addiction counselor.
Background Check
Malpractice Insurance
Every health care provider is required by law to obtain professional liability insurance to cater for the cost when found legally liable to a patient for an act in the course of his practice.
Difference Between Paneling and Credentialing
Paneling entails applying, meeting standards, and signing a contract to join a healthcare network like TRICARE. This lets providers accept network patients, increasing their patient base and revenue.
Credentialing checks a provider’s qualifications, expertise, and background to fulfill network or payer criteria. Validating licenses, education, training, and other credentials shows competence
and compliance with legislation.
Practitioners need panels to increase patient access revenue and credentialing to ensure quality care, regulatory compliance, and insurance coverage.
Paneling and credentialing affect patient attractiveness, reimbursement fee negotiation, and network access for providers. They also ensure qualified providers accept insurance, improving patient access to care.
Contact Us Today!
To become part of the TRICARE network, providers need to move through both credentialing and paneling with accuracy and consistency. Credentialing helps verify qualifications and supports quality care, while paneling helps providers expand access to covered patients.
A well-managed process can reduce delays, prevent avoidable setbacks, and make participation smoother from the start.